CARTA AL EDITOR
REVISTA DE LA FACULTAD DE MEDICINA HUMANA 2022 - Universidad Ricardo Palma10.25176/RFMH.v22i3.4984
IMPACT OF THE COVID-19 PANDEMIC IN A SPECIALIZED TUBERCULOSIS UNIT
IMPACTO DE LA PANDEMIA COVID-19 EN UNA UNIDAD ESPECIALIZADA DE TUBERCULOSIS
Xiomara Bernal-Duran2, Ángel Cubas-Alcántara2, Karina Narváez-Hidalgo2, María Navarro-Castro2, Renzo Villanueva-Villegas1-3, Félix Llanos-Tejada1-3
1 Research Professor, Instituto de Investigación de Ciencias Biomédicas, Facultad de Medicina
Humana. Universidad Ricardo Palma, Lima, Peru.
2 Student at Faculty of Human Medicine, Universidad Ricardo Palma, Lima, Peru.
3 Pulmonologist, Hospital Nacional Dos de Mayo, Lima, Peru.
Dear editor,
The COVID-19 pandemic has negatively affected other disease prevention and control programs that
could cause more deaths than the coronavirus itself (1), and also having
substantial consequences for other domains, such as social impact: slowing economic growth and
increasing rates of unemployment, poverty, and food insecurity.
The pandemic context generated a particular concern for the regular provision of health services since
human and infrastructure resources for medical care were transferred to services related to COVID-19,
for this reason, patients with health problems health not related to COVID-19 were abandoned by not
having access to health care services (2). Consequently, control measures and
epidemiological surveillance of tuberculosis (TB) were affected, which would produce an increase in the
number of cases (3).
Peru is one of the countries with the highest incidence of tuberculosis, both sensitive and resistant,
in the world. Although the public health measures adopted in the country have improved the care,
diagnosis and management of People Affected by TB (PAT), there are still limitations in the control of
the disease, especially in multidrug-resistant TB (MDR), People Deprived of Freedom (PDF) and People
Living with HIV (PLWHIV), as referred to by Guin et al. (4).
According to data from the World Bank, between 40 and 60 million people will have fallen into extreme
poverty in 2020 as a result of COVID-19, knowing the close relationship between poverty and TB, an
increase in prevalence and incidence is expected to medium and long term (1).
Both COVID-19 and TB affect the respiratory system, primarily the lungs, and have similar symptoms such
as cough, fever, and shortness of breath, although the severity and duration of symptoms vary (1). But, COVID-19 has overtaken TB as the infectious disease with the highest
death rate per day (5). Comorbidities such as chronic kidney disease,
diabetes, lung cancer, and chronic obstructive pulmonary disease (COPD), especially secondary to
smoking, have a higher risk of hospitalization and death when related to COVID-19 and/or TB (6). A preventive measure to prevent the spread of SARS-CoV-2 was mandatory
social isolation at home, however, this measure could facilitate the transmission of TB, due to
prolonged contact at home (7).
During the COVID-19 pandemic (2020-2021), in the Specialized Tuberculosis Unit of the Pulmonology
Service at Hospital Nacional Dos de Mayo, a more than double increase in the prevalence of hospitalized
patients with Type 2 Diabetes Mellitus (DM2) and TB (Figure 1) ompared to the
periods prior to the pandemic (2015-2019); which could be explained as a secondary effect of poor
control of the disease, late diagnosis and inadequate follow-up of chronic diseases, due to the
insufficient functioning of the first level of care (8).

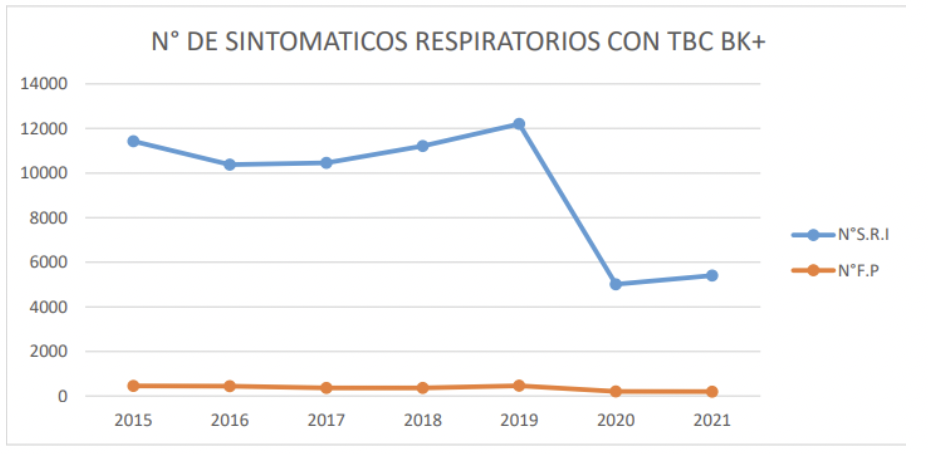
The average uptake of respiratory symptoms decreased by 46.8% during the pandemic period, compared to the pre-pandemic period (Figure 2); however, no change was found in the percentage of positive smear microscopy when we compared the period prior to the pandemic (3.7%) with the period of the pandemic (3.8%). In addition, we evidenced that there was no change in the average number of hospitalizations of patients with MDR-TB 9.
Finally, the average number of deaths hospitalized for tuberculosis increased by 60% during the pandemic (Figure 1), compared to the previous period; this would be due to the late diagnosis of the disease and hospitalization due to severe complications, such as meningoencephalitis (MEC), TB and TB with respiratory failure 10.
Today, two years after the pandemic began in Peru, the ambitious challenge is to mitigate its effects, without neglecting pre-existing diseases, especially remembering that both infections share social determinants of health, related to poverty, which today would have increased after confinement throughout Peru.
In addition, any investment made in the management of the coronavirus should be used for the care of TB patients; citing as examples effective social isolation, hand washing, and mandatory use of a mask in closed public places. Similarly, the implementation of new molecular laboratories to optimize and speed up the diagnosis of TB in the future. The current situation is radically changing the way we manage TB for the foreseeable future and unmasking vulnerabilities; it is necessary to get back on track, in order to avoid an unprecedented health crisis 11.
Author Contribution: XBD, ACA, KNH, MCN, RVV and FLT have also participated in the preparation and final approval of the letter to the editor.
Financing: Self-financed.
Declaration of conflicts of interest: Renzo Villanueva-Villegas is supported by the Fogarty Research Training Grant in Chronic Noncommunicable Respiratory Diseases in Peru (PulmPeru), funded by D43 (D43TW011502). The rest of the authors declare no conflict of interest.
Received:
Approved:
Corresponding author: Karina Narváez-Hidalgo
Adress Cipriano Rivas 524 San Juan de Miraflores, Lima - Peru
Telephone: 951807600
E-mail: karina.narvaez@urp.edu.pe
REFERENCES
