LETTERS TO THE EDITOR
DOI 10.25176/RFMH.v19.n2.2073
1 Faculty of Medicine, National University of San Agustín, Arequipa-Peru.
a Medical student.
Dear. Editor
Community-acquired pneumonia (CAP) remains a hot topic, and it is defined as an acute inflammatory disorder of lung parenchyma in patients who have acquired the infection in the community and have not been hospitalized during the past 3 weeks1.
CAP is the most lethal infectious disease in the world, and its increasing incidence is a consequence of the increment chronic diseases, immunosuppression and life expectancy. As a result, which leads to an increase in vulnerable population2.
On the other hand, heart failure (HF) along with other cardiovascular diseases (CVD) are the leading cause of death in the world3. Cardiovascular diseases rank fourth in Peru.4.
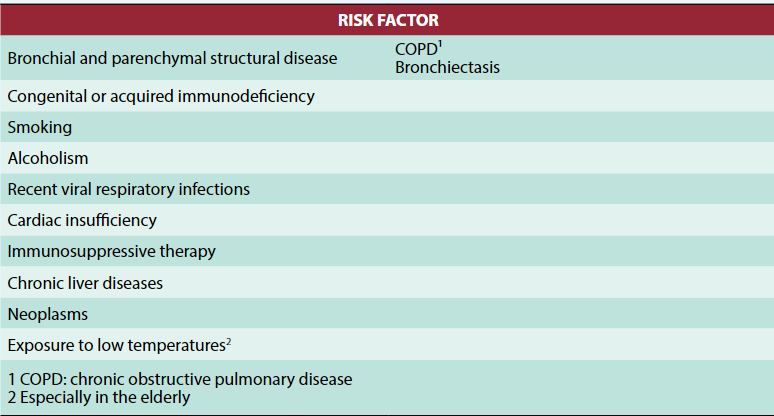
The CAP guidelines of the Peruvian Society of Infectious and Tropical Diseases states that heart failure is among the risk factors of CAP, table 11.
However, there is controversy about the direction of the causal relationship of heart failure (HF) against community-acquired pneumonia.The ambivalence is whether HF leads to immunocompromisation that offers a gateway to the infectious agents, or if CAP appears as a factor associated with the development of cardiovascular disease. Lastly, Corrales et al. suggest some repercussions of acute pneumonia in the cardiovascular system, table 25
.
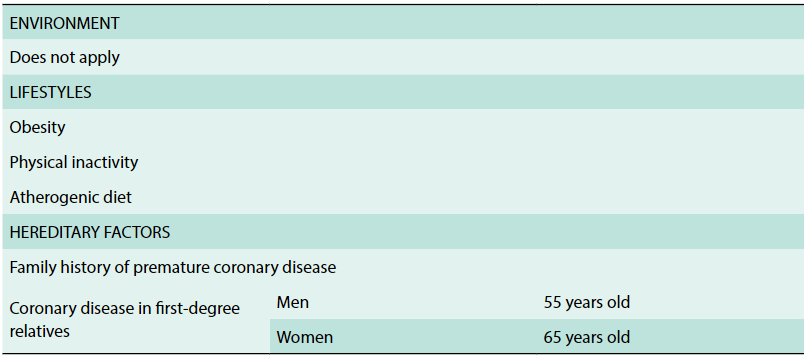
In the of 2013 cardiology clinical practice guide, published by the ministry of health, the factor of association is not considered as CI, table 36
.
A cardiovascular event in the CAP pathway gives a lousy prognosis. In a review by Cillóniz et al., it was recorded that approximately one-fifth of cases are associated with cardiovascular complications and IC is among the most common reasons for readmission7. This may be due to complications of the disease. The study of Violi et al. explain that the mortality of patients with CAP was higher (17.6%) in patients who develop CVD compared to those who did not developed CVD (4.5%)8. Although in another study, age and comorbidity were not associates to CAP in the hospitable admission. The age variable had an association with death due to the same cause9. In turn, Feldman et al. indicate that a 30% of hospitalized patients by CAP reach to develop an ECV10 . However, we talk about short- term events
A cohort study in Canada showed that community-acquired pneumonia substantially increases the risk of long-term heart failure. As a result, patients with CAP that are less than or equal to 65 years of age are 1.98 times more likely to develop HF. Unlike patients older than 65 years whose relative risk is lower. It also increases the probability of being hospitalized for an incident related to heart failure one year after discharge (RR = 1.86, 1.50 to 2.32, p <0.001)11
.
The population below 65 years is not likely to contract pneumonia in the community and to not consider pneumonia as a risk factor for HF would expose the economically active population(EAP) to cardiovascular events. This would create a greater loss of productivity in the young population due to the incidence of CVD.
It is proposed that in the next update of clinical management guidelines, pneumonia should be evaluated as a comorbidity of HF emphasizing the adult population under 65 as vulnerable in long term periods and promoting preventive strategies of the case.
