ARTICULO ORIGINAL
REVISTA DE LA FACULTAD DE MEDICINA HUMANA 2021 - Universidad Ricardo Palma10.25176/RFMH.v21i1.3408
FAMILY COHESION AND TIME OF HOSPITALIZATION IN PATIENTS WITH MENTAL DISORDERS IN A HOSPITAL IN LAMBAYEQUE, PERU
COHESIÓN FAMILIAR Y TIEMPO DE INTERNAMIENTO EN PACIENTES CON TRASTORNOS MENTALES DE UN HOSPITAL DE LAMBAYEQUE, PERÚ
Kimberly Requelme Portocarrero1, Juliana Melissa Delgado Arriola1, Alain Eduard Monsalve Mera1, Víctor Hugo Díaz Silva1,2, Ricardo Villarreal Trujillo1,3
1 Escuela de Medicina, Universidad Católica Santo Toribio de Mogrovejo. Chiclayo, Perú
2 Hospital Regional Lambayeque. Lambayeque, Perú
3 Centro especializado de salud mental comunitario. Chiclayo, Perú
ABSTRACT
Mental disorders represent about 22% of the total burden of disease, and family support plays an important role in the length of hospitalization time in these patients. We described the family cohesion and the time of hospitalization in patients of the psychiatric service of the Hospital Nacional Almanzor Aguinaga Asenjo (H.N.A.A.A) during 2019. This is a cross-sectional descriptive census-type study, in which a questionnaire of 11 questions on family cohesion was applied. Sociodemographic and clinical data were collected through a data collection form. 60 patients were surveyed, the median age was 50 years, the most frequent diagnosis was schizophrenia; most are female, not working and are single. The median length of hospitalization was 12.5 days. Those who respond positively to questions tend to stay longer.
Keywords: Psychosocial support systems, hospitalization, mental disorders. (Source: MESH – NLM)
RESUMEN
Los trastornos mentales representan cerca del 22% de la carga total de enfermedades y el apoyo familiar juega un rol importante en la duración del tiempo de hospitalización en este tipo de pacientes. Se describió la cohesión familiar y el tiempo de internamiento en los pacientes del servicio de psiquiatría del Hospital Nacional Almanzor Aguinaga Asenjo (H.N.A.A.A) durante el año 2019. Este es un estudio descriptivo transversal tipo censal, en el cual se aplicó un cuestionario de 11 preguntas sobre cohesión familiar. Se recolectaron datos sociodemográficos y clínicos a través de una ficha de recolección de datos. Se encuestaron 60 pacientes, la mediana de edad fue de 50 años, el diagnóstico más frecuente fue esquizofrenia; la mayoría son de sexo femenino, no trabaja y son solteros. La mediana del tiempo de internamiento fue 12,5 días. Los que responden de manera positiva las preguntas tienden a permanecer más tiempo internados.
Palabras Clave: Sistemas de apoyo psicosocial, hospitalización, trastornos mentales. (fuente: DeCS BIREME).
INTRODUCTION
Family is the main source of support(1) in whom we rely on in moments
of crisis and facing a mental disorder affects the family unit, meaning, what happens to one member
resonates in all the other family members.( 2) Several diverse studies exist that show that family
cohesion plays an important role as co-adjuvant in the recovery process of patients with mental
disorders(3), this favors less relapses, lower drug doses, lower symptom
severity(3) and a better quality of life(4).
Likewise, the burden and stress, of the family member or caretaker(3), in this
group of psychiatric patients, is reflected in their abandonment in public hospitals particularly in
countries with high poverty rates(2).
Family cohesion influences the time of hospital stay, since patients with socio-familiar support
are hospitalized for shorter duration(5) and have less hospital admissions in
comparison with low family cohesion(6) . Psychiatry is one of the areas that
family and social factors have more influence, becoming a protective factor for shorter duration and
lower complication of hospital stay(1), therefore, an important relationship
exists between family cohesion and hospitalization(1–5).
However, in our reality there exist few studies on mental health related to these variables,
therefore, we propose describing family cohesion and time of hospitalization in patients with mental
disorders in the psychiatry service of Hospital Almanzor Aguinaga Asenjo, Chiclayo, Peru. Moreover,
describe the psychiatric disorders of patients admitted in the psychiatry service in the year 2019,
describe family cohesion that exists in hospitalized patients in the psychiatric service, define the
average time of hospitalization in the psychiatric service and, lastly, identify the sociodemographic
aspects (sex, age, origin, educational level, diagnosis, occupation and marital status) of the patients
hospitalized in the psychiatric service.
THE STUDY
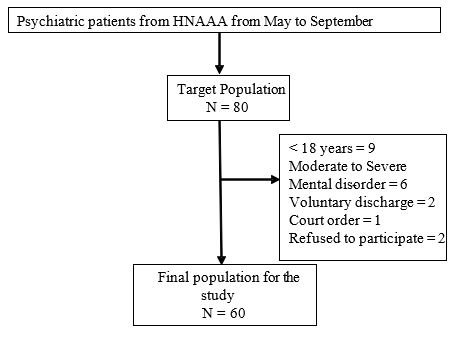
We performed a descriptive, cross-sectional study with a census sampling. The target population were 80 patients of which 60 met the inclusion criteria and 20 were excluded, 9 of which were under 18 years of age, 6 with moderate-severe mental disorder, 4 with voluntary discharge, 1 with admission per court order, and 2 refused to participate (Figure 1). They were treated between the months of May to September of 2019 in the hospitalization area of the Psychiatric Service of the H.N.A.A.A. Patients that were clinically stable were excluded, meaning fit and stable according to the evaluation performed by the medical specialist and that were under medical discharge. We did not consider patients with neurocognitive decline, those abandoned by their family, with admission per court order, under 18 years of age, with voluntary discharge and those who refused to participate in the study.
A questionnaire was used and it was made up of 11 questions, related to family cohesion, drawn
from the manual belonging to the Epidemiological Study of Mental Health in Metropolitan Lima and Callao
– 2012 edition, which was adapted and validated for the population in Lima by the Instituto Nacional de
Salud Mental Honorio Delgado – Hideyo Noguchi.(6,7) The 11
questions were validated qualitatively by three expert psychiatrists from the city of Chiclayo, who
evaluated the clarity , relevance and pertinence of each item.
We had access to clinical histories in order to obtain the duration of hospitalization,
sociodemographic data, which is information that was transcribed to the data collection sheet. Family
cohesion data was obtained from the patient interview.
All the information mentioned was stored in a data base using the Microsoft Excel 2013 version
15,0 program spreadsheet. The numeric variables were described using the median and interquartile range
through the SPSS version 25 program and the categorical variables were described as absolute and
relative rates. Tables were used for the sociodemographic and clinical variables.
We obtained the approval of the Ethics Committee of the Universidad de Santo Toribio de
Mogrovejo and of the H.N.A.A.A. The information regarding the study was offered to the patients and
their family members in case they were present. The patients that accepted to participate in the study
signed the informed consent. The study posed minimal risks given that the psychiatric patients were a
vulnerable population.
FINDINGS
60 people were surveyed, in which the family cohesion rate was searched from the psychiatric patient perspective and the hospitalization time in the psychiatric service of the H.N.A.A.A. We found that in psychiatric patients the median age was 50 years (RI: 32-58 years), the majority were of the feminine sex, almost all originating from Lambayeque, the predominant education level was complete high school and higher education. Furthermore, we found that the majority of the patients were not employed (46/60), were single (38/60), and presented schizophrenia as the most frequent diagnosis (see Table 1).
Table 1. Sociodemographic and clinical variables of the psychiatric patients from H.A.A.A.
| Sociodemographic and clinical variables | n | % |
|---|---|---|
| Sex | ||
| Feminine | 32 | 53,3% |
| Masculine | 28 | 46,6% |
| Origin | ||
| Lambayeque | 54 | 90,0% |
| Other | 6 | 10,0% |
| Educational level | ||
| Complete high school | 16 | 26,6% |
| Institute | 13 | 21,6% |
| Incomplete high school | 10 | 16,6% |
| University | 7 | 11,6% |
| Complete grade school | 4 | 6,6% |
| Incomplete grade school | 3 | 5,0% |
| Incomplete higher education | 6 | 10,0% |
| Illiterate | 1 | 1,6% |
| Diagnosis | ||
| Schizophrenia | 21 | 35,0% |
| Mild mental retardation | 4 | 6,6% |
| Bipolar disorder | 5 | 8,3% |
| Borderline personality disorder | 3 | 5,0% |
| Depression dissocial disorder | 3 | 5,0% |
| Recurrent depressive syndrome | 3 | 5,0% |
| Other | 21 | 35,0% |
| Occupation | ||
| Unemployed | 46 | 76,6% |
| Employed | ||
| Trade | 11 | 18,3% |
| Professional | 3 | 5,0% |
| Marital Status | ||
| Single | 38 | 63,3% |
| Married | 12 | 20,0% |
| Others | 10 | 16,6% |
The median of hospitalization time was 12.5 days (RIC: 8-17,7 days). Of the 60 patients, the questions that obtained greater rates were the following: for the category “a lot or very much” the questions “How much would it matter to you to embarrass your family?” (43/60), “How proud are you of your family?” (33/60), for the category “none or a little” the question “Do you feel you can count on your family when you have problems?” (22/60), and for the category “regular’ the question “How much do you feel you support one another?” (27/60) (see Table 2).
Table 2. Questions linked to family cohesion in the psychiatric patient treated in H.A.A.A.
| Questions | Nothing or little | Regular | A lot or very much |
|---|---|---|---|
| How much would it matter to you to embarrass your family? | 6 (1%) | 11 (18,3%) | 43 (71,7 %) |
| How much do you feel respected? | 17 (28,3%) | 25 (41,6%) | 18 (30%) |
| How much do you feel you support one another? | 10 (16,6%) | 27 (45%) | 23 (38,3%) |
| How proud are you of your family? | 8 (13,3%) | 19 (31,6%) | 33 (55%) |
| How much do you feel your values are similar to those of your family? | 14 (23,3%) | 24(40%) | 22(36,6%) |
| How much do you feel part of the progress of your family? | 19 (31,6%) | 23 (38,3%) | 18 (30%) |
| Do you feel you can count on your family when you have problems? | 22 (36,6%) | 15 (25%) | 23 (38,3%) |
| Do you discuss your personal issues with your family? | 20 (33,3%) | 22 (35,6%) | 18 (30%) |
| Do they take your opinion into account in important decisions? | 16 (26,6%) | 23 (38,3%) | 21 (35%) |
| Does your family show interest in your feelings? | 14 (23,3%) | 23 (38,3%) | 23 (38,3%) |
| Do you feel your family takes you into account? | 14 (23,3%) | 20 (33,3%) | 26(43,3%) |
Regarding the days of hospitalization for the questions related to family cohesion, the questions that had a higher median of hospitalization days for those that responded, “nothing or little” were the following questions: “How much would it matter to you to embarrass your family?” and “How proud are you of your family?” with a median of 15 days and of 15.5 days, respectively (Table 3).
Table 3. Hospitalization time based on questions related to family cohesion of psychiatric patients from Hospital Almanzor Aguinaga Asenjo.
| Questions | Nothing or little | Regular | A lot or very much | |||
|---|---|---|---|---|---|---|
| Median | R.I | Median | R.I | Median | R.I | |
| How much would it matter to you to embarrass your family? | 15 | 12 - 26,25 | 10 | 6 - 24 | 12 | 8 - 18 |
| How much do you feel respected? | 12 | 8 - 17 | 15 | 7 - 19,5 | 12,5 | 7,75 - 18,25 |
| How much do you feel you support one another? | 12 | 8,5 - 20 | 15 | 9 - 18 | 12 | 7 - 18 |
| How proud are you of your family? | 15,5 | 10,5 - 31,75 | 10 | 6- 19 | 13 | 8 - 17 |
| How much do you feel your values are similar to those of your family? | 10 | 8,5 - 18,75 | 14 | 6 - 18 | 14 | 8,75 - 19 |
| How much do you feel part of the progress of your family? | 10 | 7 - 17 | 17 | 8 - 24 | 15 | 7,75 - 17,25 |
| Do you feel you can count on your family when you have problems? | 10 | 6,75 - 17,75 | 12 | 8 - 17 | 15 | 9 - 19 |
| Do you discuss your personal issues with your family? | 10 | 5 - 19,25 | 14,5 | 8 - 17,25 | 14,5 | 11 - 21,5 |
| Do they take your opinion into account in important decisions? | 9,5 | 6 - 16,25 | 15 | 8 - 17 | 15 | 8,5 - 19 |
| Does your family show interest in your feelings? | 12 | 8,5 - 17, 75 | 12 | 6- 19 | 14 | 8 - 18 |
| Do you feel your family takes you into account? | 12 | 7 - 17,75 | 13,5 | 6- 19 | 14,5 | 8 - 18 |
For those who responded “a lot or very much”, the questions with a higher median of hospitalization days were the following questions: “Do you feel you can count on your family when you have problems?”, “Do they take your opinion into account in important decisions?” and “Do you feel your family takes you into account?” with a median of 15 years and 14.5days for the first two and for the last one, respectively (Table 3).
DISCUSSION
In the studied population, the median age was 50 years of age, the female gender predominated
slightly (53%), and the most frequent diagnosis was schizophrenia (35%). The average age of the studied
population was 50 years, which differs from other studies where the average age was of young adults (20
-40 years)(3,8). Likewise, the male gender predominated in
the majority of studies(3,8).
As far as similarities to other studies, the most frequent diagnosis was schizophrenia(3,8). We researched that having a psychiatric disorder
potentially affected personal achievement(9) , which could be why the majority
of patients in the current study were single, unemployed and without higher education.
The median hospitalization days in this study was 12.5 days, which is much less in comparison to
the hospitalization time of other studies whose average was 21 days(10) .
This could be because during hospitalization the focus is directed towards stabilizing acute mental
disorder symptoms and not towards a strict control of the disease during hospital stay, such as the
medical treatment follow-up after compensating the crisis and educating family members as a primary
source of support to lower patient relapse(11). Also, having been one of the
only hospitals that has exclusive hospitalization for psychiatric patients they avoid inappropriately
occupying hospital beds, which could generate pressure for an early discharge(11). Early diagnosis may also influence prolonged hospitalizations(4) since not all have the same severity, however, it is ruled out that disease
type may influence that hospitalization days be shorter here than in other hospitals, since in the
majority of studies schizophrenia diagnosis was prevalent just as in this study(3,8,9).
We found that in two questions when patients responded in a positive manner, they had lower
hospital stay. 72% (43/60) of patients cared “a lot or very much” about embarrassing their family, and
55% of patients felt proud of their family: in both questions they had less hospitalization days in
comparison to those who responded, “little or none”. Patients with psychiatric disorders feel and live
their condition, which causes them to feel blame, fear and shame for their attitude due to society
stereotypes and prejudice(12). These feelings reflect in their interaction
with society and how it affects their families’ feelings. In the same manner, the majority of patients
feel that their family does not respect them. We found that 42% of patients feel that their family
respects them in a regular manner, while 28% feel that they do not respect them. In this respect we take
into account that anyone with any psychiatric disorder is considered different in society, violating
ethical principles that prevent them from being treated with the respect they deserve(13).
Patients with interfamily support, who count on family in case they have problems and feel that
they are taken into account, remained hospitalized longer. Different studies reveal that counting on
support is an important factor for the progress of disease and less hospitalization days in a patient
with a psychiatric disorder since the family’s attitude with respect to the disorder of one of its
family members is vital for their treatment and recovery(9).
However, hospitalization days are more prolonged in patients who count on family support than in
those who responded “none or little” to the questions in the survey questionnaire. These results may be
influenced by the distortion of reality in schizophrenic patients, in whom their distorted perception
leads them to assert that they do not have a mental disorder or any problem in their lives(14)
As a limitation, despite the questionnaire used is an instrument used and adapted by the
Instituto Nacional de Salud Mental Hideyo Noguchi, we were no table to determine if the patient has
family cohesion or not, discussing the questions separately. However, the study’s importance is
highlighted for having served as a first step to evaluate how much support psychiatric patients receive
from their families and exposes the need to count on an instrument to evaluate family cohesion from the
patient and from the family member in charge.
The age median was 50 years, the female gender slightly predominated, and the most frequent
diagnosis was schizophrenia. The hospitalization time (12.5 days) was much lower than the average time
in other studies and it did not meet the psychiatric service minimum of 60 days, an established norm
under the general mental health law in Peru. The majority of patients cared about embarrassing their
family and felt proud of it. Those who responded questions in a positive manner, tended to remain
hospitalized longer than those who responded negatively.
We suggest developing an instrument to evaluate family cohesion, from the patent as well as from
the family member in charge of their care, one that may be taken as a reference for future research
considering the lack of studies in this topic.
Author contributions: The authors participated in the creation of the idea, project
design, data collection and interpretation, result analysis and manuscript preparation of the
current research study.
Financing: Self-financed.
Conflict of interests: The authors declare no conflict of interests.
Received: October 29, 2020
Approved: January 24, 2021
Correspondence: Alain Eduard Monsalve Mera.
Telephone: Av, Mariscal Nieto # 489, Chiclayo, Lambayeque - Perú
Address: +51 919 060 424
E-mail: monsalvemera@gmail.com
BIBLIOGRAPHY REFERENCES