Relationship between tacrolimus dosage and renal function, acute rejection and early infections, single center experience
Asociación entre los niveles de tacrolimus y la función renal temprana, rechazo agudo e infecciones tempranas en el trasplante renal, experiencia de un centro
Keywords:
Tacrolimus, Early graft function, Kidney transplantation, Infections, Acute rejectionAbstract
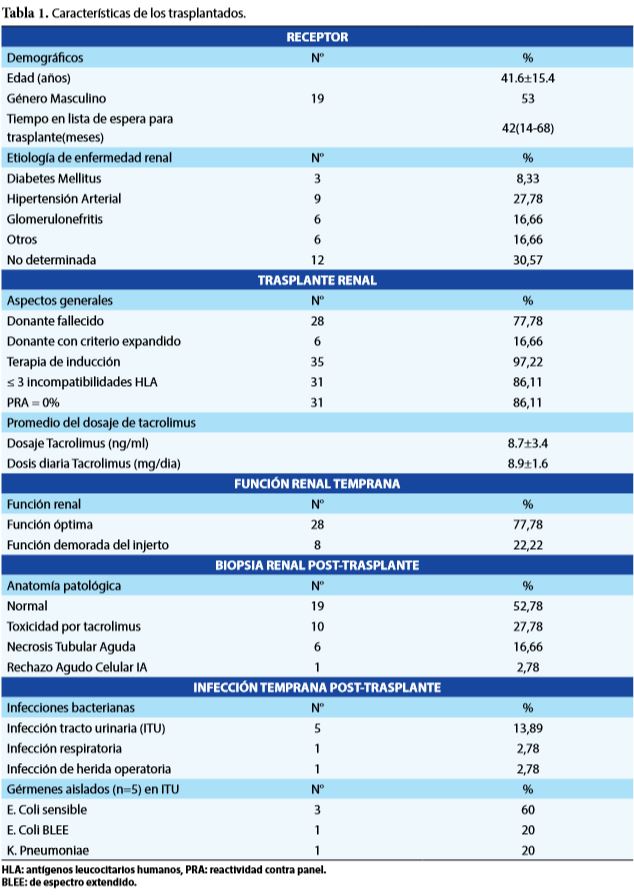
Objectives: The aim was to determine the association between tacrolimus levels and early renal graft function, acute rejection and infections in the first month after early kidney transplantation. Methods: Retrospective, observational and analytical study. Review of records of kidney transplant patients over 18 years of age during 2016, who met the inclusion criteria (n = 36). The descriptive and analytical statistics were with STATA 15, significance p <0.05. Results: Age 41.6 ± 15.3, males 52.78%, deceased donor 77.78%, 86.11% had ≤ 3 incompatibilities HLA and PRA 0%. They received induction 97.22%. Tacrolimus dose (TAC C) on the seventh day was 8.7 ± 3.4 ng / ml. The 16.66% were donors of expanded criteria, 22.22% with delayed graft function, acute tubular necrosis (6/36), anticalcineurin toxicity (10/36) and acute cellular rejection IA (1/36). The overall TAC C / D ratio <1.05 was calculated. The frequency of infections was 19.45%, the most frequent urinary infection being 13.85% with 20% E.coli BLEE. There is a relationship between the level of tacrolimus> 12 ng / ml on the seventh day and the presence of infections at the first month post-renal transplantation (p <0.05). There was no relationship between tacrolimus levels with renal function, acute rejection, HLA incompatibilities and induction (p> 0.05). Conclusion: The level of Tacrolimus on the seventh day post-transplant> 12ng / ml was associated with early infections a month after renal transplantation. Key words: Tacrolimus; Early graft function; Kidney transplantation; Infections; Acute rejection. (source: MeSH NLM)
DOI: 10.25176/RFMH.v18.n2.1282
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2018 Revista de la Facultad de Medicina Humana

This work is licensed under a Creative Commons Attribution 4.0 International License.